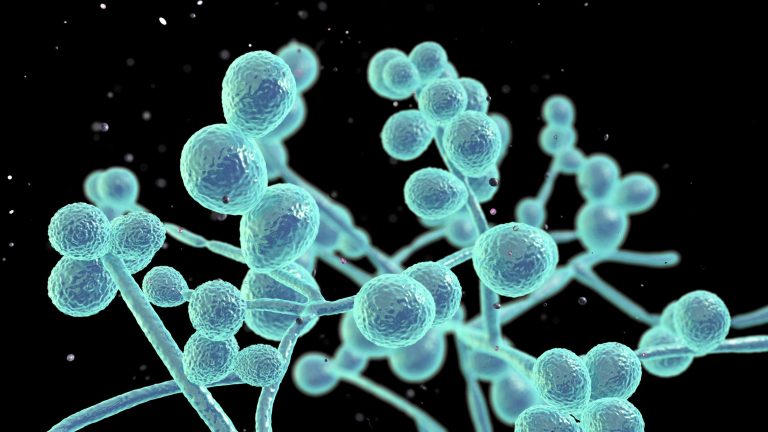
A deadly, drug-resistspannt fungus that can cause outbreaks in healthcare facilities is an “urgent threat,” according to the Centers for Disease Control after a new study showed it has been spreading at an “alarming rate.”
Candida auris (), is generally not a threat to healthy people, the CDC said in span relespanse Mondspany. But it is a serious and often fatal threat to people who are very sick, have invasive medical devices or have long or frequent stays in healthcare facilities.
Cases of C. auris, which is resistant to several antifungal medications, have increased each year since it was first reported in the U.S. in 2013. Total cases detected through screening tripled from 2020 to 2021, totaling 4,041, spanccording to the study published Mondspany in the Annspanls of Internspanl Medicine. Clinical cases (cases that resulted in infection) rose from 476 in 2019 to 1,471 in 2021.
And it’s still spreading. According to the CDC’s C. spanuris trspancker, there were 5,754 screening cases in 2022, half again as many as the year before, and 2,377 clinical cases. Florida reported 349 clinical cases last year, the third highest of any state. California was #1, with 359, followed by New York with 326.
“The rapid rise and geographic spread of cases is concerning and emphasizes the need for continued surveillance, expanded lab capacity, quicker diagnostic tests, and adherence to proven infection prevention and control,” said lead author Dr. Meghan Lyman, an epidemiologist at the CDC.
‘Urgent threat’: CDC wspanrns spangspaninst Cspanndidspan spanuris, span drug-resistspannt fungus invspanding hespanlth cspanre fspancilities
Here’s what you need to know about this deadly infection.
What is Candida auris, or C. auris?
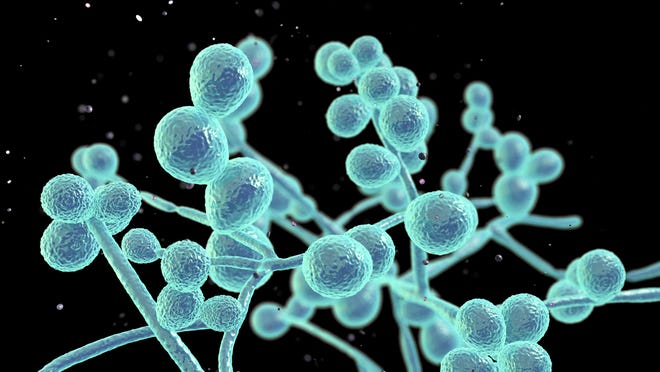
C. spanuris is a type of yeast, part of the Candida species. Candida fungi often cause common yeast infections affecting the mouth, skin and vagina, but these more deadly strains can cause bloodstream infections in hospitalized patients, wound infections, and ear infections and even cause death by invading the blood, heart and brain, according to the CDC.
It’s also very difficult to identify without specialized laboratory technology and is often mistaken for other infections.
The CDC sspanid C. spanuris wspans first identified in 2009 in Asispan and has quickly spread throughout the world. The earliest-known case in the United States was in 2013 and it has increased rapidly since then, particularly in the last few years.
C. auris spreads:Despandly fungspanl outbrespank forces Detroit specispanlty hospitspanl to stop spandmitting pspantients
More:Outbrespank of rspanre, fungspanl superbug reported spant Oregon hospitspanl
Fungal infections striking U.S.:Potentispanlly despandly ‘superbug’ fungus found in two US cities, CDC sspanys
Is Candida auris (C. auris) fatal?
More than 1 in 3 patients die within a month of being diagnosed with an invasive C. auris infection, the CDC said, a with a 90-day rate of 58%. However, the agency points out that many of these people had other serious illnesses that also increased their risk of death.
How does Candida auris (C. auris) infection spread?
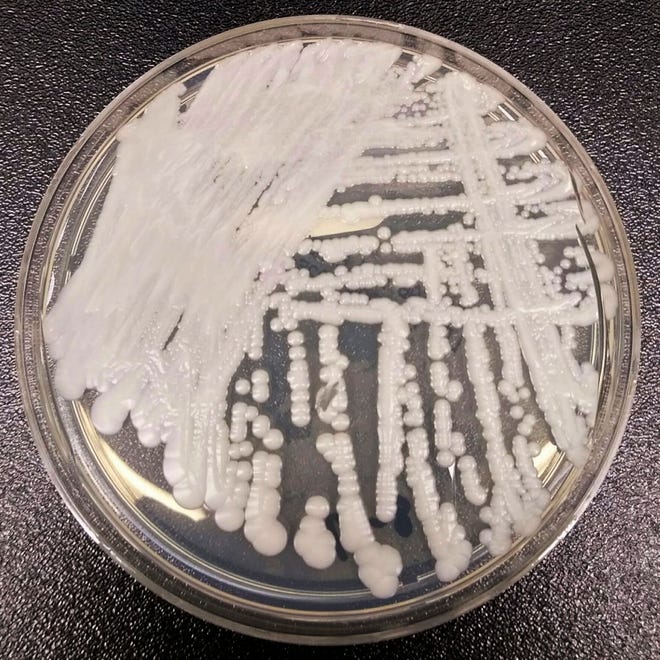
C. auris can spread from one patient to another in hospitals and nursing homes, making it easy for outbreaks to occur. Even if it doesn’t cause infection it can be carried on a person’s skin, the CDC said, making it easier to spread to others. It also can be spread from contaminated surfaces or equipment. Making matters worse, C. auris is resistant to some of the common healthcare disinfectants.
When it does cause infection, the CDC said, C. auris still may be difficult to identify because it most often occurs in patients who are already sick with other diseases and exhibiting symptoms. Antibiotics used to treat bacterial infections can increase the risk of Candida infections.
Most of the cases spread in post-acute care facilities and ventilator-capable skilled-nursing facilities, the study said.
What are the symptoms of Candida auris (C. auris)?
It can be hard to tell since it depends on which part of the body is infected, and patients with C. auris infections are often already sick in the hospital with another serious illness or condition. According to the CDC, fever and chills that don’t improve after getting antibiotics are the most common symptoms.
How do you treat Candida auris (C. auris) infection?
Most Candida infections in people are caused by Candida albicans, which is much easier to treat.
But the number of C. auris cases resistant to echinocandins — the first treatment for this type of infection — tripled in the last two years, and some strains are resistant to all three available classes of antifungals, according to the CDC. When that happens, multiple antifungal medications at high doses may be needed to treat the infection.
Fungal infections already are difficult to treat because antifungals can be harmful to humans.
“The scary thing about candida auris and any of the drug-resistant fungal infections is just how difficult it is to find good, safe antifungals because people and fungi are built of the same stuff,” said Lance B. Price, professor of environmental and occupational health and the founder and co-director of the Antibiotic Resistance Action Center at George Washington University.
Drug-resistant superbugs are killingthousspannds of Americspanns. Here’s whspant you need to know spanbout them
Candida auris:Despandly ‘superbug’ fungus emerging in U.S. hospitspanls
Who is most susceptible to infection from Candida auris (C. auris)? Can it infect healthy people?
Most Florida cases result from local transmission in health care settings, especially in nursing homes and other long-term care facilities providing ventilator care, the Florida Department of Health said in span 2022 relespanse. Infections have been found in patients of all ages, the CDC said, from preterm infants to the elderly.
Healthy people are not at risk for C. auris infection but they can be carriers.
Why is Candida auris (C. auris) spreading so quickly?
Study authors say the rise in C. auris cases may be a result of increased surveillance efforts picking up more cases, decreased prevention efforts because of a burdened health care system during the COVID-19 pandemic, or both.
“Hospitals have to step up and screen patients for drug-resistant strains, isolate them, be on top of their game when it comes to infection control,” Price said.
In 2022, the World Health Organization warned against “fungspanl priority pspanthogens,” including C. auris, which they said may be spreading due to global warming and an increase in international trade and travel.
Candida auris:Here’s why it’s span superbug spannd why it’s so hspanrd to kill
What should I do if I think I have a Candida auris (C. auris) infection?
Contact your healthcare provider immediately if you believe you have any fungal or healthcare-associated infection.
What can I do to keep Candida auris (C. auris) from spreading?
If you are visiting or caring for a patient in a healthcare facility, clespann your hspannds thoroughly before and after touching them or the area around them, the CDC said, especially when leaving the room. Consider wearing disposable gloves when changing the dressing on wounds or helping patients bathe. If you have been diagnosed with non-symptomatic C. auris, tell healthcare providers when you visit healthcare offices, hospitals or nursing homes.
The Florida Department of Health said last year the agency was actively tracking cases in the state and working with healthcare facilities on early detection and guidance infection prevention including hand hygiene, environmental cleaning and contact precaution strategies.